Changing minds about Alzheimer's
Protecting against memory and behaviour changes
Approximately 46 million people worldwide are living with dementia, and every three seconds someone is diagnosed with the condition. Now researchers at Southampton show that regulating immune cells in the brain could prevent memory loss and behaviour changes seen in the progression of Alzheimer’s disease.
Alzheimer’s is a big problem in today’s ageing population, as it affects a lot more people than just those diagnosed with the chronic condition. The disease has an impact on the family and carers, and on the economy. It is a huge burden on healthcare providers, explains Dr Diego Gomez-Nicola, Associate Professor within the School of Biological Sciences at the University.
New thinking
Diego and his team are studying a relatively new strand of research into Alzheimer’s – the role of inflammation in the progression of the disease, which was pioneered by professors Hugh Perry and Clive Holmes, both working at Southampton. They showed that when a person with Alzheimer’s has some kind of inflammation such as a cold or infection, the disease worsens.
Southampton is the best place to study the role of inflammation on the neurobiology of Alzheimer’s disease. We have a really good link between basic and clinical research, an excellent background in the role of inflammation in degenerative diseases, and access to clinical samples
“Our research focuses on cells called microglia: the main immune cells of the brain. When too many of these cells are produced, inflammation is caused in the brain and therefore the disease is accelerated.”
Their work published in recent years, funded by the Medical Research Council (MRC) and Alzheimer’s Research UK, used tissue samples from healthy brains and those with Alzheimer’s, both of the same age. By counting the number of microglia in both samples, the team found that they were more numerous in the brains with Alzheimer’s. In addition, the activity of the molecules regulating the numbers of microglia correlated with the severity of the disease.
Improve cognitive skills
“We have studied the microglia in different mouse models, which have different aspects of Alzheimer’s. We wanted to find out whether blocking the receptor responsible for regulating microglia, known as CSF1R, could improve cognitive skills,” explains Diego.
The team gave the mice oral doses of an inhibitor that blocks CSF1R and found that it could prevent the rise in microglia numbers seen in untreated mice as the disease progressed. In addition, the inhibitor prevented the loss of communication points between the nerve cells in the brain associated with Alzheimer’s, and the treated mice demonstrated fewer memory and behavioural problems compared with the untreated mice.
“Importantly, we found the healthy number of microglia needed to maintain normal immune function in the brain was preserved, suggesting the blocking of CSF1R only reduces excess microglia,” says Diego.
“In the last few years, scientists in Southampton have been at the forefront of research into the role of the immune system in Alzheimer’s, so it is encouraging to see this study taking these ideas forward by identifying a specific mechanism that could be a target for future treatments,” said Dr Simon Ridley, Director of Research at Alzheimer’s Research UK.
Our role is to design and test better inhibitors for CSF1R with the aim of developing better drugs with a profile that more specifically targets the brain
Collaborating for success
By working in collaboration with external partners, the next step is to use the findings to improve the lives of people with Alzheimer’s disease. Diego and his team are part of the Dementia Consortium, a collaboration between Alzheimer’s Research UK, LifeArc and pharmaceutical companies Eisai, Lilly and AbbVie.
The team are also part of the Wellcome Trust Immunology Consortium. Half of the consortium focuses on research into Alzheimer’s and the other half is studying mood disorders, explains Diego. “We liaise with industrial partners such as GSK, Pfizer, Lundbeck and Johnson & Johnson to investigate whether commercially available drugs that are licenced for other diseases, could be used to target brain inflammation and therefore be repurposed for use against Alzheimer’s.” As a result of this collaboration, an inhibitor to block microglial proliferation will be tested in patients with mild cognitive impairment (MCI) from 2018.
Diego hopes that in five years’ time progress from these two initiatives could mean the research is closer to clinical trials. “The mouse models are promising, but we don’t know what the impact is on the human set up. With clinical trials we would be able to monitor the microglia with imaging technology over time to confirm the impact on the cognitive output.”
Find out more about Dr Diego's research
You may also be interested in:

Tackling public health challenges
Instigating step changes in public health, both in the UK and internationally.
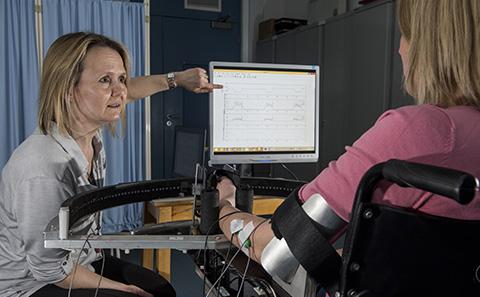
Enabling stroke rehabilitation
Southampton researchers are developing innovative solutions to help people recover from stroke.
Getting under the skin of allergies
Our researchers are leading the largest study of its kind to improve our understanding of allergies
