Clinician scientists based at the Centre for Cancer Immunology have shown a rare form of cancer can be treated with a drug thatŌĆÖs already available on the NHS.
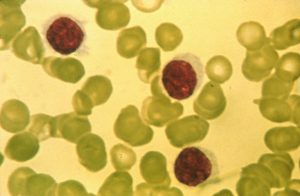
Hairy Cell Leukaemia (HCL) is a chronic leukaemia and gets its name from the tiny, hair-like projections on the cellŌĆÖs surface. Current treatment is usually chemotherapy which has many side effects and does not eradicate the disease completely.
Professor Francesco Forconi, professor of Haematology at the University of Southampton and haematologist at University Hospital Southampton NHS Foundation trust, observed that HCL have mechanisms, making the hairy cells unable die, but can specifically be targeted by Venetoclax, a drug already used to treat other blood cancers and has fewer side effects. He has treated the first HCL patient with this drug.
Professor Forconi hopes the case, which has been published in the New England Journal of Medicine (NEJM) will open conversations between the pharma industry, clinicians and clinical trial specialists and lead to more studies in HCL patients.
David Halford, from Southampton, was diagnosed with HCL in 2007 after he felt unwell. ŌĆ£I thought I had a chest infection,ŌĆØ he said. ŌĆ£But has soon as the doctor saw me, he sent me straight to hospital. I was shocked when they told me it was cancer. I just wanted to go home, but they wouldnŌĆÖt let me. I had to have an immediate blood transfusion before starting the chemotherapy. I just kept thinking ŌĆśhow long have I got?ŌĆÖ It was so scary.ŌĆØ
David had several rounds of chemotherapy which put the disease under control for some time but had a lot of side effects including sickness and extreme fatigue. He had to have six months off being a postman, a job he loves and has now done for 29 years.
In 2018 however, David began to feel unwell again and scans revealed the cancer had returned. This time, David did not want chemotherapy and Professor Forconi proposed Venetoclax.
He explained: ŌĆ£Patients with HCL are usually treated with a type of chemotherapy called purine analogues, but it can be toxic and does not eradicate the disease completely. Patients can also benefit from specific inhibitors of BRAF, a protein that helps HCL cells grow. However, these are not available on the NHS and even when they are used, again they do not kill the disease completely.
ŌĆ£Venetoclax works by blocking another protein in HCL called Bcl2, which protects the cancer cells from being destroyed. Venetoclax stops Bcl2 from working and kills the cells. Importantly, it does this with very little side effects for the patient. We were thrilled to see it work so well in David.ŌĆØ
After just five weeks of taking Venetoclax in tablet form, David was feeling much better, and amazingly tests showed he was in remission, which meant he could go back to his post rounds.
ŌĆ£I couldnŌĆÖt believe it,ŌĆØ David said. ŌĆ£I thought I would have to have another six months off work, but it was absolutely amazing to be back after five weeks. The experience was completely different to the treatment before. I hardly experienced any side effects. The treatment was brilliant as were all the medical staff at the hospital. They are wonderful people who work so hard.ŌĆØ
The University of Southampton is an international centre of excellence for HCL. Together with Ohio State University and Royal Marsden Hospital, Southampton researchers are developing a registry on HCL to enable researchers to study HCL in ways not previously possible given the rarity of the disease. The registry will collect patient data and help researchers identify new trends in patient outcomes, discover previously unknown complications of the disease, and design clinical trials for new therapies until a cure is discovered.
Professor Forconi added: ŌĆ£David was an excellent example of showing how we can use other drugs to treat rare diseases. I hope that our ongoing conversations between pharma and clinicians will lead to meaningful plans to do more research and clinical trials into how we can help people with this rare form of cancer.ŌĆØ