Immobilisation of the cervical spine with a cervical collar (c-collar) is routine care for trauma patients until potential fractures or ligamentous injury are ruled out (American College of Surgeons, 2008). Additionally, c-collars are frequently applied for longer durations to provide restrictions in cervical range of motion (ROM) during community rehabilitation (Webber-Jones, 2002). In order to limit cervical mobility, collars are fixed securely to the individual’s neck via strapping and height adjustment, creating points of increased pressure and shear forces at the skin-device interface. Coupled with an altered microclimate, resulting from increased interface temperature and humidity, these devices pose a high risk for pressure ulcers (PU) development. Patients requiring c-collars are vulnerable to skin damage due to their reduced ability to sense and respond to noxious stimuli, including pressure, owing to reduced consciousness or neurological deficit.
Prevalence of c-collar related tissue breakdown has been reported to range from 6.8-38% and documented as high as 55% when worn for greater than 5 days
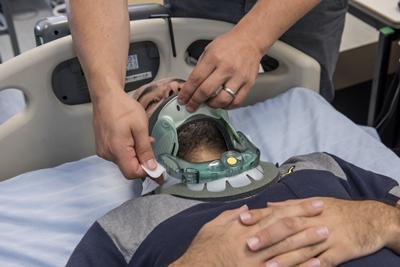
Common sites of skin breakdown specifically associated with c-collars include the occiput, mandible, ears, chin, laryngeal prominence, shoulders and sternum (Hewitt, 1994). Many trauma patients, especially critically ill individuals, have increased susceptibility to PUs, potentially resulting from reduced consciousness (Ham et al,. 2014a), response to noxious stimuli (Bader et al., 2005) and reduced intrinsic tolerance to pressure (Buchanan et al,. 1987). Prevalence of c-collar related tissue breakdown has been reported to range from 6.8-38% (Ham et al,. 2014b) and documented as high as 55% when worn for greater than 5 days (Davis et al,. 1995). However, much of the existing literature regarding c-collars consists of observational studies (Davis et al,. 1995; Powers et al,. 2006) concerned with PU incidence.
There is a need to monitor the physiological reaction of the skin during c-collar application. Recent research investigating skin health has identified inflammatory cytokines as suitable biomarkers to monitor the physiological response of skin to pressure and shear. Experimental studies have been conducted to investigate the effects of device strap tension on microclimate, interface pressure and the physiological inflammatory response of the skin tissue (Worsely et al, 2016). However, this experimental approach has not yet been applied to c-collars, despite the unacceptably high incidence of collar-related PUs.
The proposed work package will investigate the effects of varying c-collar design and application technique on tissue interface pressure, microclimate (temperature and humidity) and the physiological response of the skin at the skin-device interface. In particular we will investigate the influence of materials used within the c-collars regarding their compliance with the skin and ability to allow airflow to vulnerable skin tissues.
Refs
American College of Surgeons Committee on Trauma. Advanced Trauma Life Support for Doctors. 8thed. Chicago: American College of Surgeons Committee on Trauma; 2008
Webber-Jones JE, Thomas CA, Bordeaux RE, Jr. The management and prevention of rigid cervical collar complications. Orthop Nurs 2002;21:19-25; quiz -7.
Hewitt S. Skin necrosis caused by a semi-rigid cervical collar in a ventilated patient with multiple injuries. Injury 1994;25:323-4.
Ham HW, Schoonhoven LL, Galer AA, et al. Cervical collar-related pressure ulcers in trauma patients in intensive care unit. J Trauma Nurs 2014;21:94-102.
Bader DL, Bouten C, Colin D. Pressure ulcer research: current and future perspectivesed: Springer Science & Business Media, 2005.
Davis JW, Parks SN, Detlefs CL, et al. Clearing the cervical spine in obtunded patients: the use of dynamic fluoroscopy. J Trauma 1995;39:435-8.
Powers J, Daniels D, McGuire C, et al. The incidence of skin breakdown associated with use of cervical collars. J Trauma Nurs 2006;13:198-200.
Worsley PR, Prudden G, Gower G, Bader DL. Investigating the effects of strap tension during non-invasive ventilation mask application: a combined biomechanical and biomarker approach. Medical Devices Evidence and Research. 2016; 9; 409-417