Professionalism touches on every aspect of medical students’ training and doctors’ practice. The GMC makes several recommendations for medical students about professionalism (see Tomorrow's Doctors) from doctors, medical students, and patients perspectives. Professionalism is sometimes presented (and assessed) as a matrix of different competences that students need to develop and be able to demonstrate.
It includes:
- Being able to perform competently (and being aware of your limitations of competence) as befits the different stages of your training
- Awareness of what is required for, and how to record, your professional development
- Understanding your professional responsibility and how you are regulated
- Knowing where to access support and how to request assistance and supervision as appropriate
- Being able to work with others, their teachers and as part of a team
- Understand how their own wellbeing and resilience influences their work
- Giving and receiving feedback and knowing how to ask for help and recognising when it is required
- Establishing the foundations of continuous personal and professional development
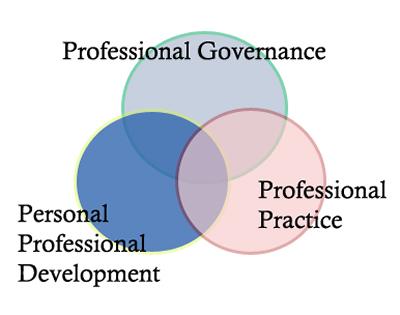
Professionalism is about more than how you behave in practice. It includes the attitudes and values you hold and that run through the profession as a whole. At Southampton we consider the different issues and responsibilities relating to Professionalism in three main areas:
- Professional Governance issues related to collective responsibility as part of a profession such as regulatory and management issues. To include a knowledge and ability to contribute to and understand where and how discussions and decisions are made about broader issues of Health Policy. Also an understanding of how an individual's professional development and career fits into the provision of health care more generally.
- Professional Practice issues related to clinical practice including the doctor / patient relationship and the delivery of care. This includes how to act professionally in clinical settings and within a number of different situations a student is likely to meet in practice.
- Personal Professional issues related to a student's own professional development including their wellbeing, their personal professional development and identifying when and how to access support.
Issues that emerge for students within the university and in clinical attachments often mirror the issues they will come across once they have completed their training.
Students need to understand how their careers are likely to develop and feel empowered and informed to influence their career progression. Governance encompasses, but is not exclusively about, aspects of student progress and disciplinary work.
Students at Southampton are frequently supported through problems, either formally by academic, personal or pastoral tutors, or informally perhaps from peer support or other channels. How students that do not access the formal support network deal with difficulties that relate to their professional development is not always clear, although this may mirror the variety of ways different doctors handle the diverse professional challenges they face.
It has been suggested that during a student's undergraduate years, time should be set aside for reflecting upon and developing professional values, as well as learning a set of personal behaviours in clinical settings. The Royal College of Physicians report on medical professionalism suggested that:
- Professionalism will only be valued and fostered by proper attention to its place in medical education.
- Education has a critical part to play in strengthening the ethos of professionalism.
- Education about professionalism will provide a far better way to improve the standard of patient care than any regulatory regime.
Doctors have responsibilities to their patients, employers and those who contract their services. This means that doctors are both managers and are managed.
All doctors work in systems and within organisations that have a direct and far-reaching impact on patient experience and outcomes. Doctors have a legal duty broader than any other health professional and therefore have an intrinsic leadership role with in healthcare services. They have a responsibility to contribute to the effective running of the organisation in which they work and to its future direction.
The development of leadership competence is an integral part of a doctor's training and learning. The NHS Next Stage Review Final Report, issued by the Department of Health in 2008, highlighted the need for all doctors to be practitioners, partners and leaders. The report stated: 'Greater freedom, enhanced accountability and empowering staff are necessary but not sufficient in the pursuit of high quality care.'
Making change actually happen takes leadership. It is central to our expectations of the healthcare professionals of tomorrow. There may be other ways for students to achieve a greater understanding of the purpose of regulation, the procedures of the regulators and the role this will play in their professional careers. One option could be to require teaching on these issues in all pre-registration professional education and training.
Reference: 'Trust, Assurance and Safety'. Department of Health. England (2007).
Teaching about professional issues related to patient care and management can be appropriately linked with specific interventions and offered where ever students are taught.
While many aspects of professional practice are covered and linked to clinical attachments, other broader issues that require integration during a students training are covered by and taught through the themes that influence teaching throughout the students' training.
Doctors must be capable of regularly taking ultimate responsibility for difficult decisions in situations of clinical complexity and uncertainty, drawing on their scientific knowledge and well developed clinical judgement. The doctor's role must be defined by what is in the best interest of patients and of the population served.
We provide students with the time, space and support to understand explore the rational and implications on them of the professional codes of conduct which guide the medical profession. We support and encourage students to identify and work through the issues that arise for them during their training as an essential foundation for their on-going professional development.
In the early years there are a number of facilitated sessions exploring subjects such as Doctor (and student) wellbeing and resilience, learning styles, study skills and the interplay between values, attitudes and behaviours. Students are also supported to reflect on and learn from what they find most challenging, developing the ability to use and grow from reflection, feedback and supervision.
Working with individuals and small groups on such subjects presents different challenges to teaching factual information and clinical skills. Examples of areas that students are encouraged to look at as part of their personal professional development include, learning from mistakes, working in teams, dealing with difficult situations, balancing studies and other aspects of student life, the importance of monitoring their personal wellbeing.
The General Medical Council in their guidance, 'Medical students: professional values and fitness to practice', states: "Students must be aware that their behaviour outside the clinical environment, including in their personal lives, may have an impact on their fitness to practice. Their behaviour at all times must justify the trust the public places in the medical profession."
In the GMC's publication, 'Good Medical Practice', the principles and values on which good practice are founded are set out. It states that: "You must make sure your conduct at all times justifies your patient's trust in you and public's trust in the profession." Students need time to digest this principle and reflect on its current and future implications.